This image was created with Biorender.com
A decade ago, a novel immunotherapy ravaged two pounds of cancer cells and revolutionized the treatment of blood cancer. This immunotherapy isolated T cells from a patient and inserts a gene encoding synthetic chimeric antigen receptor (CAR) ex-vivo into T cells. These CARs contain regions to redirect T cells to the targeted tumor cells and enhance T cell activity towards it. Once infused into the patient, these CAR T cells patrol the circulatory system to eradicate cancer cells. And this is how scientists cured all blood cancers in the world – at least in my imaginary world.
Currently, in the real world, CAR T cell therapy is a laborious personalized treatment that can exceed $1 million in cost. Therefore, it would be tremendously valuable to program CAR T cells in-vivo rather than collecting each patient’s own T cells and modifying them in a lab. A new approach involving messenger RNA (mRNA) may offer a more affordable use of CAR T cell therapy in the future.
Rurik and colleagues used a murine model of heart disease to assess the efficacy of the novel mRNA-based CAR T cells. In this mouse model, fibroblast cells secreted excessive protein fibers that resulted in fibrosis and impaired heart function. The therapeutic target was to eliminate the overactive fibroblast cells with the CAR T cells. Just like the Moderna and Pfizer mRNA COVID-19 vaccine technology, the researchers used lipid nanoparticles (LNP) as a shuttle for the mRNA. The LNPs are designed to deliver the cargo specifically to T cells by recognizing their unique surface marker. On arrival, the cargo mRNAs are released into the cytoplasm, where they are translated into a CAR that recognizes fibroblast activation protein (FAP). As their name suggests, FAPs are found on the surface of activated fibroblasts that contribute to fibrosis.
The scientists took the LNP-encapsulated mRNA (LNP-mRNA) on a test drive in a T cell culture. The LNP-mRNA delivery system successfully instructed 83% of the T cells to express FAP-specific CAR (FAPCAR). Encouraged by the result, the scientists then evaluated the therapeutic potential of LNP-mRNA by testing it in mice with heart disease. When these mice received the LNP-mRNA treatment, approximately 20% of their T cells are transformed into FAPCAR T cells. The FAPCAR T cell army consists of both CD4+ helper and CD8+ killer T cells. This dynamic duo would act in concert to launch a robust attack against their shared targets – in this case, the overactive fibroblast. And voila! The mice were ridden of their fibrosis and now had restored heart functions! In fact, when scientists assessed these hearts histologically, the treated mice looked no different than the completely healthy ones!
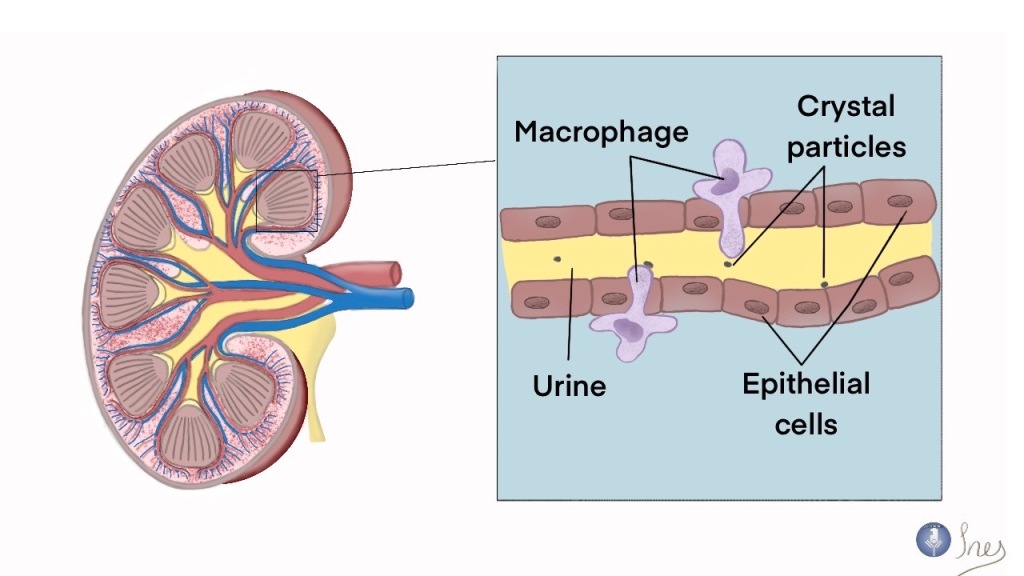
Microscopic examination revealed these LNP-mRNA based CAR T cells nibble on the surfaces of their target cells in a process known as trogocytosis. This observation is consistent with the activity of earlier gene-based CAR T cell therapy, which further attests to the functionality of the in-vivo generated CAR T cells.
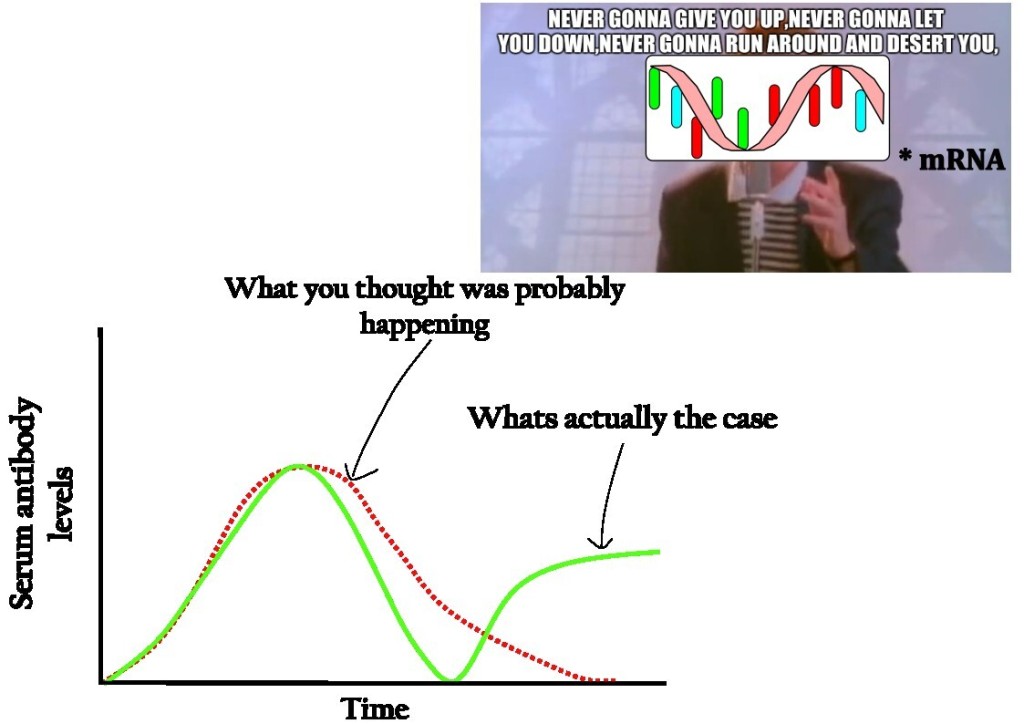
The efficacy of FAPCAR T cells in the mouse model provides promising evidence for LNP-mRNA based CAR T cell technology. The transient nature of mRNA brings more opportunities for dosing control and may lead to new applications of CAR T cell therapy. Additionally, the well-established safety of mRNA COVID-19 vaccines serves as a promising precedent for the LNP-mRNA based CAR T cell technology. If successful in human trials, this novel technology may have significant implications for the accessibility of CAR T therapy. Just like the LNP-mRNA COVID-19 vaccines, the novel CAR T manufacturing process may be upscaled, made more affordable and widely available!
Source:

Article author: YongGuang Jiang. Yong is an IRTA postbaccalaureate fellow at the National Institute of Health. His research is focused on studying the role of plasmin and neutrophil elastase in hematopoietic recovery.
Editor: Sutonuka Bhar. Sutonuka is a PhD candidate at the University of Florida. Her work focuses on host immune responses against viruses and bacterial membrane vesicles.
Check out Antibuddies’ blog post “A step towards affordable cell therapy using mRNA technology”.
Tweet



Leave a comment